PHILADELPHIA – A novel protein marker has been found that identifies rare adult liver stem cells, whose ability to regenerate injured liver tissue has the potential for cell-replacement therapy. For the first time, researchers at the University of Pennsylvania School of Medicine led by Linda Greenbaum, MD, Assistant Professor of Medicine in the Division of Gastroenterology, have demonstrated that cells expressing the marker can differentiate into both liver cells and cells that line the bile duct.
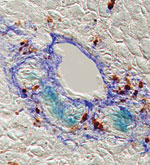 |
Liver stem cells expressing FoxL1 (aqua blue) in an injured mouse liver near the bile duct. The FoxL1-containing stem cells are encircled by liver fibroblasts (royal blue), suggestive of a stem cell niche.
Click on thumbnail
to view full-size image |
In the future, this marker will allow for the isolation and expansion of these stem cells, which could then be used to help patients whose livers can no longer repair their own tissue. About 17,000 Americans are currently on a waiting list for a liver transplant, according to the American Liver Foundation. The findings appear online this month in the journal Hepatology.
“In a healthy liver, proliferation of mature liver and bile-duct lining cells is sufficient to maintain the necessary size and function of the organ,” explains Greenbaum. “This even works when the liver is confronted with mild and acute injury, but the situation changes when injury to the liver is chronic and severe.”
For chronic injury, the liver uses a back-up system that stimulates stem cells to proliferate and eventually differentiate into new liver cells. Greenbaum and colleagues found that these dual-potential stem cells can be identified and potentially isolated from other liver cells because they uniquely express the protein Foxl1. The team showed that in two mice models of liver injury, stem cells and their descendents were marked by the expression of FoxL1. The researchers propose to use this marker to isolate the Foxl1-bearing stem cells and transplant them back into damaged livers to restore function.
“At this point, we haven’t identified the molecular targets that are regulated by Foxl1 in the liver stem cell,” says Greenbaum. The researchers also do not yet know what signals activate the expression of Fox l1 and how exactly it is related to liver function. But, they finally have a molecular handle on identifying liver stem cells, which have remained elusive to scientists.
“This work has significant implications for cell-replacement therapies of chronic liver disease in the future,” says Greenbaum.
Sara Sackett, Zhaodong Li, Reginald Hurtt, Yan Gao, Rebecca Wells, Karrie Brondell, and Klaus Kaestner, all of Penn, are co-authors. The University of Pennsylvania Institute for Regenerative Medicine and the Penn Center for Digestive Diseases Center (Grant P30DK50306) provided funding for this research.
###
PENN Medicine is a $3.6 billion enterprise dedicated to the related missions of medical education, biomedical research, and excellence in patient care. PENN Medicine consists of the University of Pennsylvania School of Medicine (founded in 1765 as the nation's first medical school) and the University of Pennsylvania Health System.
Penn's School of Medicine is currently ranked #4 in the nation in U.S.News & World Report's survey of top research-oriented medical schools; and, according to most recent data from the National Institutes of Health, received over $379 million in NIH research funds in the 2006 fiscal year. Supporting 1,700 fulltime faculty and 700 students, the School of Medicine is recognized worldwide for its superior education and training of the next generation of physician-scientists and leaders of academic medicine.
The University of Pennsylvania Health System (UPHS) includes its flagship hospital, the Hospital of the University of Pennsylvania, rated one of the nation’s top ten “Honor Roll” hospitals by U.S.News & World Report; Pennsylvania Hospital, the nation's first hospital; and Penn Presbyterian Medical Center. In addition UPHS includes a primary-care provider network; a faculty practice plan; home care, hospice, and nursing home; three multispecialty satellite facilities; as well as the Penn Medicine Rittenhouse campus, which offers comprehensive inpatient rehabilitation facilities and outpatient services in multiple specialties.
Penn Medicine is one of the world’s leading academic medical centers, dedicated to the related missions of medical education, biomedical research, excellence in patient care, and community service. The organization consists of the University of Pennsylvania Health System and Penn’s Raymond and Ruth Perelman School of Medicine, founded in 1765 as the nation’s first medical school.
The Perelman School of Medicine is consistently among the nation's top recipients of funding from the National Institutes of Health, with $550 million awarded in the 2022 fiscal year. Home to a proud history of “firsts” in medicine, Penn Medicine teams have pioneered discoveries and innovations that have shaped modern medicine, including recent breakthroughs such as CAR T cell therapy for cancer and the mRNA technology used in COVID-19 vaccines.
The University of Pennsylvania Health System’s patient care facilities stretch from the Susquehanna River in Pennsylvania to the New Jersey shore. These include the Hospital of the University of Pennsylvania, Penn Presbyterian Medical Center, Chester County Hospital, Lancaster General Health, Penn Medicine Princeton Health, and Pennsylvania Hospital—the nation’s first hospital, founded in 1751. Additional facilities and enterprises include Good Shepherd Penn Partners, Penn Medicine at Home, Lancaster Behavioral Health Hospital, and Princeton House Behavioral Health, among others.
Penn Medicine is an $11.1 billion enterprise powered by more than 49,000 talented faculty and staff.