(PHILADELPHIA) — Researchers at
the Perelman School of Medicine are harnessing
two new, non-invasive techniques to look more closely inside the
working lungs – leading to early detection of diseases, like
emphysema, before it becomes evident in other modes of imaging.
“Up until now, imaging the way lungs function in real time
has been limited by conventional methods which result in rather
low resolution images,” comments Warren
Gefter, MD, Chief
of Thoracic
Imaging in the Radiology
Department at Penn. “We
are developing a way to get a better look inside the lungs by polarizing atoms -- making them all spin in the same direction -- with magnetic
resonance [MR], which allows the atoms to have a strong signal
for sharper images.”
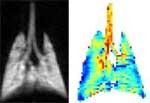 |
Images of lung function using hyperpolarized
helium
Click on thumbnail
to view full-size image |
Hyperpolarized 3He gas allows radiologists to observe the
lung as gas flows in and out, giving them high resolution images
of human ventilation. Combining several techniques enables researchers
to measure the rate of diffusion of these helium gas molecules,
which reflect the size of the air
sacs in the lung. This, in turn,
allows researchers to detect very early emphysema, even before
it’s evident on CT (computed
tomography) – providing
physicians with additional information in which to make diagnoses
and offer treatment.
Gefter adds, “We have moved from imaging the structure to
imaging the function of the lung to a scale well below a millimeter
in size. It’s truly groundbreaking.”
To use this extremely powerful research tool, which provides accurate
and precise measurements, patients must inhale the helium at the
exact right time, after it’s been exposed to a laser light
to make all of the atoms spin in the same direction, creating the
polarized helium, which then enters the lung.
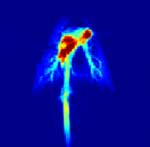 |
MRI of animal lung using polarized carbon-13
Click on thumbnail
to view full-size image |
Utilizing another new MR technique, Penn imaging researchers are
pushing the scale of what we see in the lung down to an even smaller
level -- to the cellular and intracellular level. Investigators
have figured out a way in which they hope to look for a “marker” of
disease inside the body. In animal models, they are injecting polarized
carbon-13-labeled molecules and watching its conversion in real
time. They can take images of the carbon-13 as it shuffles through
the metabolic steps inside the cell.
Rahim Rizi, PhD, Associate Professor of Radiology at Penn, explains, “We
observe the polarized carbon-13 labeled molecule as it breaks down
and releases energy. What this ‘flagged molecule’ converts
into could tell us whether the cell is normal or abnormal. This
is a whole new approach to molecular imaging. For the first time,
we can now follow the C-13 molecule, in real time, as it moves
throughout the body to pinpoint the location of disease. It’s
real-time molecular imaging. This is revolutionary to MRI technology.”
Penn is one of only a few sites in the world, and the only site
on the East Coast, with this capability. Penn researchers hope
to translate this technique for use in humans before the end of
2007.
Editor's Note: The National
Institutes of Health funded this research work, with additional aid by General
Electric.
###
PENN Medicine is a $2.9 billion enterprise
dedicated to the related missions of medical education, biomedical
research, and high-quality patient care. PENN Medicine consists
of the University of Pennsylvania School of Medicine (founded in
1765 as the nation's first medical school) and the University of
Pennsylvania Health System.
Penn's School of Medicine is ranked #2 in the nation for receipt
of NIH research funds; and ranked #3 in the nation in U.S. News
& World Report's most recent ranking of top research-oriented
medical schools. Supporting 1,400 fulltime faculty and 700 students,
the School of Medicine is recognized worldwide for its superior
education and training of the next generation of physician-scientists
and leaders of academic medicine.
The University of Pennsylvania Health System includes three hospitals,
all of which have received numerous national patient-care honors [Hospital
of the University of Pennsylvania; Pennsylvania Hospital, the nation's
first hospital; and Penn Presbyterian Medical Center]; a faculty practice
plan; a primary-care provider network; two multispecialty satellite
facilities; and home care and hospice.
Penn Medicine is one of the world’s leading academic medical centers, dedicated to the related missions of medical education, biomedical research, excellence in patient care, and community service. The organization consists of the University of Pennsylvania Health System and Penn’s Raymond and Ruth Perelman School of Medicine, founded in 1765 as the nation’s first medical school.
The Perelman School of Medicine is consistently among the nation's top recipients of funding from the National Institutes of Health, with $550 million awarded in the 2022 fiscal year. Home to a proud history of “firsts” in medicine, Penn Medicine teams have pioneered discoveries and innovations that have shaped modern medicine, including recent breakthroughs such as CAR T cell therapy for cancer and the mRNA technology used in COVID-19 vaccines.
The University of Pennsylvania Health System’s patient care facilities stretch from the Susquehanna River in Pennsylvania to the New Jersey shore. These include the Hospital of the University of Pennsylvania, Penn Presbyterian Medical Center, Chester County Hospital, Lancaster General Health, Penn Medicine Princeton Health, and Pennsylvania Hospital—the nation’s first hospital, founded in 1751. Additional facilities and enterprises include Good Shepherd Penn Partners, Penn Medicine at Home, Lancaster Behavioral Health Hospital, and Princeton House Behavioral Health, among others.
Penn Medicine is an $11.1 billion enterprise powered by more than 49,000 talented faculty and staff.