PHILADELPHIA – University of Pennsylvania School of Medicine researchers have discovered how the expression of the Sonic hedgehog gene is regulated during brain development and how mutations that alter this process cause brain malformations. The results appear online this month in Nature Genetics.
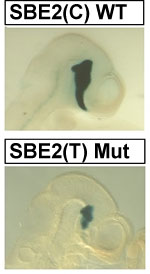 |
Comparison of expression of a reporter gene under the regulatory control of a wild type and mutant Shh brain enhancer - SBE2 (blue). Note that the reporter gene is expressed more fully from the wild type (WT) versus the mutant (Mut) Shh enhancer in the hypothalamus of a 10-day-old mouse embryo.
Credit: Douglas J. Epstein, University of Pennsylvania School of Medicine
|
Sonic hedgehog (Shh) plays a key role in regulating many aspects of embryonic development including, growth of digits on limbs and organization of neurons in the brain. It controls cell division of adult stem cells and has been implicated in some cancers.
"Elucidating the regulators of Shh expression in the forebrain will not only improve our fundamental understanding of brain development, but may also lead to novel insights into the pathogenesis of holoprosencephaly and possibly other malformations in the brain,” says senior author Douglas J. Epstein, PhD, Associate Professor of Genetics.
Holoprosencephaly occurs when an embryo's forebrain, the large frontal area of the human brain, fails to divide to form left and right halves, causing defects in the development of the face and in brain structure and function. Symptoms can be moderate, in the case of a cleft lip or palate to severe, as in cyclopia, the development of one eye rather than two. About one in 16,000 live births display a type of holoprosencephaly.
A decrease in the Shh protein by 50 percent predisposes humans to craniofacial problems such as holoprosencephaly. Too much Shh can lead to tumor formation. Shh is the most commonly mutated gene in holoprosencephaly and can involve about seven other genes.
In a previous study published in the journal Development, the Penn group surveyed one million bases, the basic building blocks of DNA, in transgenic mice for the sequences that turn on Shh during the development of the forebrain. They identified a brain specific enhancer that drives expression of Shh in the hypothalamus. Enhancers are regulatory sequences that drive a gene’s transcription, ensuring that it is turned on and off at the appropriate time. Enhancers can be located nearby to the genes they regulate or, as in the case of Shh, operate over hundreds of thousands of base pairs away.
In the current study, the investigators searched for mutations in the enhancer sequence in holoprosencephalic patients. They identified one mutation in a region of the enhancer that has been conserved for over 300 million years of evolution, attesting to the importance of these sequences. The mutation caused a significant reduction in Shh enhancer activity in the hypothalamus.
In turn, they screened for proteins that assemble on the Shh brain enhancer. They found a protein called Six3 that binds less tightly to the mutated form of the Shh enhancer. The enhancer can’t work without the proteins that bind to it, and this study showed a direct link between the Six3 DNA- binding protein, the sequence that regulates Shh, and hence brain development. Interestingly, mutations in Six3 also cause holoprosencephaly, but the mechanism by which this occurs was previously unknown. Results from the Penn study now indicate that it is likely through the failure to activate Shh.
Identifyng additional components of the Shh brain enhancer complex will further our understanding of how gene regulatory networks operate during normal brain development. This type of basic research should also be instrumental in identifying additional causes of holoprosencephaly and other congenital brain anomalies resulting from the misregulation of Shh expression.
Penn coauthors are Yongsu Jeong and Federico Coluccio Leskow. This research was funded in part by an NIH grant from the National Institute of Neurological Disease and Stroke (NINDS) and a grant from the March of Dimes.
###
PENN Medicine is a $3.6 billion enterprise dedicated to the related missions of medical education, biomedical research, and excellence in patient care. PENN Medicine consists of the University of Pennsylvania School of Medicine (founded in 1765 as the nation's first medical school) and the University of Pennsylvania Health System.
Penn's School of Medicine is currently ranked #4 in the nation in U.S.News & World Report's survey of top research-oriented medical schools; and, according to most recent data from the National Institutes of Health, received over $379 million in NIH research funds in the 2006 fiscal year. Supporting 1,700 fulltime faculty and 700 students, the School of Medicine is recognized worldwide for its superior education and training of the next generation of physician-scientists and leaders of academic medicine.
The University of Pennsylvania Health System (UPHS) includes its flagship hospital, the Hospital of the University of Pennsylvania, rated one of the nation’s top ten “Honor Roll” hospitals by U.S.News & World Report; Pennsylvania Hospital, the nation's first hospital; and Penn Presbyterian Medical Center. In addition UPHS includes a primary-care provider network; a faculty practice plan; home care, hospice, and nursing home; three multispecialty satellite facilities; as well as the Penn Medicine Rittenhouse campus, which offers comprehensive inpatient rehabilitation facilities and outpatient services in multiple specialties.
Penn Medicine is one of the world’s leading academic medical centers, dedicated to the related missions of medical education, biomedical research, excellence in patient care, and community service. The organization consists of the University of Pennsylvania Health System and Penn’s Raymond and Ruth Perelman School of Medicine, founded in 1765 as the nation’s first medical school.
The Perelman School of Medicine is consistently among the nation's top recipients of funding from the National Institutes of Health, with $550 million awarded in the 2022 fiscal year. Home to a proud history of “firsts” in medicine, Penn Medicine teams have pioneered discoveries and innovations that have shaped modern medicine, including recent breakthroughs such as CAR T cell therapy for cancer and the mRNA technology used in COVID-19 vaccines.
The University of Pennsylvania Health System’s patient care facilities stretch from the Susquehanna River in Pennsylvania to the New Jersey shore. These include the Hospital of the University of Pennsylvania, Penn Presbyterian Medical Center, Chester County Hospital, Lancaster General Health, Penn Medicine Princeton Health, and Pennsylvania Hospital—the nation’s first hospital, founded in 1751. Additional facilities and enterprises include Good Shepherd Penn Partners, Penn Medicine at Home, Lancaster Behavioral Health Hospital, and Princeton House Behavioral Health, among others.
Penn Medicine is an $11.1 billion enterprise powered by more than 49,000 talented faculty and staff.