PHILADELPHIA – Researchers at the University of Pennsylvania School of Medicine have discovered stem cells in the esophagus of mice that were able to grow into tissue-like structures and when placed into immune-deficient mice were able to form parts of an esophagus lining. The investigators report their findings online this month in the Journal of Clinical Investigation.
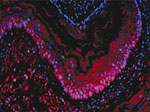 |
Mouse esophagus stem cells have the capacity to contribute to the repair of esophageal epithelium after induction of injury.
Click on thumbnail
to view full-size image |
“The immediate implication is that we’ll have a better understanding of the role of these stem cells in normal biology, as well as in regenerative and cancer biology,” says senior author Anil K. Rustgi, MD, the T. Grier Miller Professor of Medicine and Genetics and Chief of Gastroenterology. “Down the road, we will develop a panel of markers that will define these stem cells and use them in replacement therapy for diseases like gastroesophogeal reflux disease [GERD] and also to understand Barrett’s esophagus, a precursor to esophageal adenocarcinoma and how to reverse that before it becomes cancer.”
Diseases of the esophagus are very common in the United States and worldwide. “Benign forms include GERD and millions are affected,” notes Rustgi.
GERD can sometimes lead to inflammation of the esophagus, called esophagitis. “In some of these cases esophagitis can lead to a swapping of the normal lining of the esophagus with a lining that looks more like the intestinal lining and that’s called Barrett’s esophagus,” explains Rustgi. “This can lead to cancer of the esophagus, which is the fastest rising cancer in the US, increasing by 7 to 8 percent a year.”
The researchers set out to identify and characterize potential stem cells--those with the ability to self renew--in the esophagus to understand normal biology and how injured cells may one day be repaired.
First, they grew mouse esophageal cells they suspected were adult stem cells. Those cells formed colonies that self renewed. These cells then grew into esophageal lining tissue in a three-dimensional culture apparatus. “These tissue culture cells formed a mature epithelium sitting on top of the matrix,” says Rustgi. “The whole construct is a form of tissue engineering.”
The investigators then tested their pieces of esophageal lining in whole animals. When the tissue-engineered patches were transplanted under the skin of immunodeficient mice, the cells formed epithelial structures. Additionally, in a mouse model of injury of the esophagus in a normal mouse, which mimics what happens during acid reflux, green-stained stem cells migrated to the injured lining cells and co-labeled with the repaired cells, indicating involvement of the stem cells in tissue repair and regeneration.
Eventually the researchers will develop genetically engineered mouse models to be able to track molecular markers of esophageal stem cells found in a micorarray study. The group has already developed a library of human esophageal cell lines and is looking for human versions of markers already identified in mice.
“The ultimate goal is to identify esophageal stem cells in a patient, grow the patient’s own stem cells, and inject them locally to replace diseased tissue with normal lining,” says Rustgi.
Penn co-authors are Jiri Kalabis, Kenji Oyama, Takaomi Okawa, Hiroshi Nakagawa, Carmen Z. Michaylira, Douglas B. Stairs, and J. Alan Diehl (Department of Cancer Biology), as well as Jose-Luiz Figueiredo and Umar Mahmood from Massachusetts General Hospital, Molecular Center for Imaging Research, Boston, and Meenhard Herlyn, from The Wistar Institute, Philadelphia.
This work was funded by the National Institute of Diabetes and Digestive and Kidney Diseases and the National Cancer Institute.
PENN Medicine is a $3.6 billion enterprise dedicated to the related missions of medical education, biomedical research, and excellence in patient care. PENN Medicine consists of the University of Pennsylvania School of Medicine (founded in 1765 as the nation's first medical school) and the University of Pennsylvania Health System.
Penn's School of Medicine is currently ranked #4 in the nation in U.S.News & World Report's survey of top research-oriented medical schools; and, according to most recent data from the National Institutes of Health, received over $379 million in NIH research funds in the 2006 fiscal year. Supporting 1,700 fulltime faculty and 700 students, the School of Medicine is recognized worldwide for its superior education and training of the next generation of physician-scientists and leaders of academic medicine.
The University of Pennsylvania Health System (UPHS) includes its flagship hospital, the Hospital of the University of Pennsylvania, rated one of the nation’s top ten “Honor Roll” hospitals by U.S.News & World Report; Pennsylvania Hospital, the nation's first hospital; and Penn Presbyterian Medical Center. In addition UPHS includes a primary-care provider network; a faculty practice plan; home care, hospice, and nursing home; three multispecialty satellite facilities; as well as the Penn Medicine Rittenhouse campus, which offers comprehensive inpatient rehabilitation facilities and outpatient services in multiple specialties.
Penn Medicine is one of the world’s leading academic medical centers, dedicated to the related missions of medical education, biomedical research, excellence in patient care, and community service. The organization consists of the University of Pennsylvania Health System and Penn’s Raymond and Ruth Perelman School of Medicine, founded in 1765 as the nation’s first medical school.
The Perelman School of Medicine is consistently among the nation's top recipients of funding from the National Institutes of Health, with $550 million awarded in the 2022 fiscal year. Home to a proud history of “firsts” in medicine, Penn Medicine teams have pioneered discoveries and innovations that have shaped modern medicine, including recent breakthroughs such as CAR T cell therapy for cancer and the mRNA technology used in COVID-19 vaccines.
The University of Pennsylvania Health System’s patient care facilities stretch from the Susquehanna River in Pennsylvania to the New Jersey shore. These include the Hospital of the University of Pennsylvania, Penn Presbyterian Medical Center, Chester County Hospital, Lancaster General Health, Penn Medicine Princeton Health, and Pennsylvania Hospital—the nation’s first hospital, founded in 1751. Additional facilities and enterprises include Good Shepherd Penn Partners, Penn Medicine at Home, Lancaster Behavioral Health Hospital, and Princeton House Behavioral Health, among others.
Penn Medicine is an $11.1 billion enterprise powered by more than 49,000 talented faculty and staff.