PHILADELPHIA –Researchers at the University of Pennsylvania School of Medicine have identified a protein from a most unlikely source -- baker’s yeast -- that might protect against Parkinson’s disease. More than a million Americans suffer from Parkinson's disease, and no treatments are available that fundamentally alter the course of the condition. By introducing the yeast protein Hsp104 into animal models of Parkinson’s disease, researchers prevented protein clumping that leads to nerve cell death characteristic of the disorder.
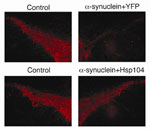 |
Red staining shows the levels of an enzyme involved in dopamine synthesis in the region of the rat brain most affected in Parkinson's disease.
Click on thumbnail
to view full-size image |
“Yeast express a protein called Hsp104, which is able to reverse protein aggregation,” says James Shorter, PhD, Assistant Professor of Biochemistry and Biophysics. “However, for reasons that are unclear, Hsp104 is not found in mammals. We wondered if introducing Hsp104 into mammals could help with diseases connected with protein aggregation.”
These findings will be published in the September 2008 issue of The Journal of Clinical Investigation and appeared online August 14, 2008.
Clinicians do not fully understand the process and cause of Parkinson’s disease. However, researchers believe that a protein called alpha-synuclein misfolds and clumps in many forms of the disease, and that this process is intimately tied to the selective death of dopamine-producing neurons that results in Parkinson’s disease.
In this study, researchers found that Hsp104 could partially reverse alpha-synuclein aggregation in test-tube experiments. Remarkably, rats expressing Hsp104 showed lower levels of alpha-synuclein aggregation and alpha-synuclein-induced toxicity of neurons. This result is significant because the rat model used recreates the selective loss of dopamine-producing nerve cells in the region of the brain affected in Parkinson’s disease, say the investigators.
“This study represents an important preliminary step,” says Shorter. “One thing we’d like to do next is to treat an animal model which already has considerable quantities of alpha-synuclein aggregates to see if Hsp104 can actually reverse the process in the rat brain.”
Co-authors in addition to Shorter are Christophe Lo Bianco of the Wallenberg Neurosciences Center in Lund, Sweden and the Brain Mind Institute in Lausanne, Switzerland; Etienne Regulier, Hilal Lasheul, and Patrick Aebischer, also of the Brain Mind Institute; Takeshi Iwatsubo at the University of Tokyo; and Susan Lindquist of the Whitehead Institute for Biomedical Research, Cambridge, MA. The Michael J. Fox Foundation, European Molecular Biology Organization, Swedish Parkinson’s Foundation, Swiss National Science Foundation, American Heart Association, University of Pennsylvania Institute on Aging, and the National Institute of Health Director’s New Innovator Award provided funding for this research.
###
PENN Medicine is a $3.5 billion enterprise dedicated to the related missions of medical education, biomedical research, and excellence in patient care. PENN Medicine consists of the University of Pennsylvania School of Medicine (founded in 1765 as the nation's first medical school) and the University of Pennsylvania Health System.
Penn's School of Medicine is currently ranked #4 in the nation in U.S.News & World Report's survey of top research-oriented medical schools; and, according to most recent data from the National Institutes of Health, received over $379 million in NIH research funds in the 2006 fiscal year. Supporting 1,400 fulltime faculty and 700 students, the School of Medicine is recognized worldwide for its superior education and training of the next generation of physician-scientists and leaders of academic medicine.
The University of Pennsylvania Health System includes three hospitals — its flagship hospital, the Hospital of the University of Pennsylvania, rated one of the nation’s top 10 “Honor Roll” hospitals by U.S.News & World Report; Pennsylvania Hospital, the nation's first hospital; and Penn Presbyterian Medical Center — a faculty practice plan; a primary-care provider network; two multispecialty satellite facilities; and home care and hospice.
Penn Medicine is one of the world’s leading academic medical centers, dedicated to the related missions of medical education, biomedical research, excellence in patient care, and community service. The organization consists of the University of Pennsylvania Health System and Penn’s Raymond and Ruth Perelman School of Medicine, founded in 1765 as the nation’s first medical school.
The Perelman School of Medicine is consistently among the nation's top recipients of funding from the National Institutes of Health, with $550 million awarded in the 2022 fiscal year. Home to a proud history of “firsts” in medicine, Penn Medicine teams have pioneered discoveries and innovations that have shaped modern medicine, including recent breakthroughs such as CAR T cell therapy for cancer and the mRNA technology used in COVID-19 vaccines.
The University of Pennsylvania Health System’s patient care facilities stretch from the Susquehanna River in Pennsylvania to the New Jersey shore. These include the Hospital of the University of Pennsylvania, Penn Presbyterian Medical Center, Chester County Hospital, Lancaster General Health, Penn Medicine Princeton Health, and Pennsylvania Hospital—the nation’s first hospital, founded in 1751. Additional facilities and enterprises include Good Shepherd Penn Partners, Penn Medicine at Home, Lancaster Behavioral Health Hospital, and Princeton House Behavioral Health, among others.
Penn Medicine is an $11.1 billion enterprise powered by more than 49,000 talented faculty and staff.