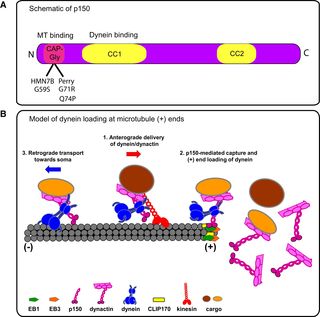
The CAP-Gly domain of p150 subunit of dynactin is required for initiation of dynein loading at plus ends. Cronin & Schwartz, Neuron, Vol. 74: 2, pp 211-213.
It never ceases to amaze me how news about the rare has the potential to inform the common. Researchers from the lab of
Erika Holzbaur, PhD,
study molecular motors -- proteins that function as tiny molecular machines to move cargos within a cell. For the last few years, Holzbaur, a professor of Physiology at the Perelman School of Medicine, University of Pennsylvania, has been using live-cell imaging to get a better handle on what happens when the transport of cellular cargo goes off track, and how that may be the start of neurodegenerative diseases. In this case, a Parkinson’s-like disorder and a hereditary form of motor neuron disease (MND).
In a recent study published in Neuron, Holzbaur and graduate student, Armen Moughamian, studied mutations in the molecular motor cofactor dynactin that are associated with Perry syndrome, an extremely rare, inherited neurodegenerative disease. Parkinson’s disease-like symptons and psychiatric changes are the predominant features of this syndrome. The dynactin complex is conserved from yeast to humans, and mutations in it not only cause Perry syndrome, but also cause a form of MND, called distal hereditary motor neuropathy 7B.
This motor neuron disease and Perry syndrome are completely distinct diseases and do not share common symptoms. Yet, amazingly, both of these diseases are caused by mutations in a single part, or domain, of dynactin called the CAP-Gly domain.
Moughamian and Holzbaur approached the problem of understanding how these distinct mutations cause two different neurodegenerative diseases by first understanding the normal function of the CAP-Gly domain of dynactin. They used live-cell imaging techniques developed in the Holzbaur lab to observe the transport of cargo in primary neurons with and without the CAP-Gly domain of dynactin. They saw no difference in movement of lysosomes, a dynactin cargo, in the neuron.
But, if there are no changes in movement, what is the CAP-Gly domain needed for and how do mutations in it affect human health?
Moughamian and Holzbaur continued to study dynactin and showed that the CAP-Gly domain is necessary to make sure dynactin does its job of getting transport started at the far end of an axon. This defect in transport ultimately causes less efficient movement in the cell, resulting in less lysosomes returning to the cell center over time.
What’s more, Moughamian and Holzbaur show that the disease-causing mutations disrupt how dynactin is shaped, making it less able to bind to cellular tracks. Moughamian and Holzbaur again used live-cell imaging techniques to show that the Perry syndrome and motor neuron disease mutations differentially disrupt transport in the neurons. The motor neuron disease mutations disrupt movement throughout the neuron, while the Perry syndrome mutations only disrupt the start of transport.
Their research suggests that mutations in the CAP-Gly domain of dynactin disrupt the normal formation of the molecular motor and its cargo, which leads to a faulty transport of the cargo and, over time, neurodegeneration.
What Moughamian and Holzbaur found reveals a novel function for the dynactin complex and paves the way for a better understanding into how distinct disrupts in transport can cause specific neurodegenerative diseases. These findings on rare diseases could potentially shed light on the pathology of more common forms of Parkinson’s and motor neuron disease.
 Moughamian AJ, & Holzbaur EL (2012). Dynactin is required for transport initiation from the distal axon. Neuron, 74 (2), 331-43 PMID: 22542186
Moughamian AJ, & Holzbaur EL (2012). Dynactin is required for transport initiation from the distal axon. Neuron, 74 (2), 331-43 PMID: 22542186